Bacterial meningitis acts fast: What may start as mild, cold-like symptoms can turn into a life-threatening situation in less than 24 hours. Ultimately, the disease — which is most common in teens, as well as infants and the elderly — kills about one in six people who develop it, and 20% survivors live with enduring side effects, such as hearing loss, according to the World Health Organization.
That’s why it’s so important to be familiar with the symptoms of meningitis. Being able to recognize early signs of the condition and get help right away can make a huge difference in survival rates. Our experts break down meningitis, including what causes it, the red flags symptoms everyone should know, and the best prevention techniques.
What Is Meningitis?
“Meningitis, in general terms, is a severe infection involving the brain,” says Sharon Nachman, M.D., chief of pediatric infectious diseases at Stony Brook Children’s Hospital.
The brain and spinal cord are covered by delicate membranes called meninges. Between the brain and spinal cord and the meninges, there’s fluid known as cerebrospinal fluid. Meningitis occurs when an infectious agent such as a virus or bacteria gets into the cerebrospinal fluid and causes inflammation in the meninges, explains William Schaffner, M.D., a professor of infectious diseases at the Vanderbilt University Medical Center.
That swelling can create pressure inside the skull and affect blood flow, leading to headaches, fevers, confusion, loss of consciousness, and seizures, according to the National Library of Medicine.
“[Meningitis] can be a milder or a much more severe infection, depending upon the nature of the infectious agents,” Dr. Schaffner says.
What Are the Types of Meningitis?
Meningitis can be caused by viruses or bacteria, and more rarely fungi or parasites, the World Health Organization reports.
Over half of meningitis cases are viral, according to the National Library of Medicine. “The viruses usually produce a transient infection that heals itself. These infections are, relatively speaking, mild,” Dr. Schaffner says.
Bacterial meningitis can be much more severe. It requires treatments, and even if cured can leave patients with “substantial disabilities,” Dr. Schaffner says. And this is the type that targets teens and young adults (as well as infants and the elderly), per the Meningitis Research Foundation.
The good news is that bacterial meningitis is relatively rare. In 2006, about 22% of all meningitis cases were caused by bacterial infections, according to the National Library of Medicine research. But since then bacterial meningitis has become less common, thanks in part to the development of vaccines that protect people from the disease, a 2025 study in The Lancet Regional Health shows.
Many different bacteria can cause bacterial meningitis. “Meningococcal meningitis is the most common form of bacterial meningitis in adolescents and young adults. [It] is caused by a bacterium called Neisseria meningitidis,” says Patti Wukovits, BSN, RN, AMB-BC, the co-executive director of the American Society for Meningitis Prevention and Executive Director of the Kimberly Coffey Foundation.
“Neisseria meningitidis lives harmlessly in the back of the nose and throat of roughly 10 to 35% of the population at any given time. In most people, the immune system keeps it contained. But in some, and we still don’t fully understand why, the bacteria breach the blood-brain barrier, enter the bloodstream, and trigger a very serious, potentially deadly infection,” Wukovits says.
What Are the Symptoms of Bacterial Meningitis?
One reason bacterial meningitis is so dangerous is because it moves very quickly. “Many initial symptoms are mild and are similar to most illnesses: headache, fever, feeling unwell,” Dr. Nachman says. “However, these symptoms rapidly progress to severe illness.” In one The Lancet study of children and teens under age 16 with the condition, most had non-specific symptoms in the first four to six hours of infection, but were close to death by 24 hours.
She says later symptoms of bacterial meningitis include:
- An inability to stand or walk
- A red or purplish pinprick rash
- High fevers
- Unresponsiveness
- A severely stiff neck that may impede movement
- A headache that progressively worsens
- Light sensitivity
- Trouble answering questions or confusion.
Viral meningitis can cause similar symptoms. According to the National Library of Medicine, these include:
- A fever
- A headache
- Sensitivity to light
- Neck stiffness
- Nausea and vomiting.
While people with bacterial meningitis will get worse over time, those with viral meningitis typically recover. But since bacterial meningitis is so severe and fast-acting, it’s not safe to wait and see how symptoms progress before seeking help.
What Should You Do If You Think Your Teen Has Meningitis?
Bacterial meningitis is rare, so unless there’s an outbreak going on in your area, early symptoms can go overlooked. But any delay in treatment can be devastating. “Call 911 or get to an emergency room immediately. Do not wait to see if they improve. Do not wait for a doctor’s appointment in the morning. This is one of the very few diseases where hours, sometimes minutes, can make a very big difference,” Wukovits says.
Specifically, Dr. Schaffner says that if your teen ever complains of a severe headache and fever of about 101 or higher at the same time, it’s a good idea to visit the doctor and ask about meningitis. If there’s a known outbreak in your area, any sign of illness at all is enough of a reason to at least call your doctor, if not go to the emergency room.
A purplish rash that doesn’t fade when you press a glass against it is also a red flag to visit the ER, Wukovits says. That said, not everyone develops one and it can be harder to see on darker skin tones, Dr. Schaffner says. So the absence of a rash can’t be taken as reassurance, especially when other symptoms of meningitis are present.
The bottom line is that since bacterial meningitis is so dangerous, it’s never a bad idea to act quickly, even if you’re not entirely sure whether the symptoms you’re noticing are signs of the condition. “[Speak] with a medical provider if your child is not acting the way they usually do. Very often the right answer is being urgently evaluated by a trusted medical provider,” Dr. Nachman says. Wukovits agrees: “Trust your gut. If something feels terribly wrong, act on that feeling.”
How Is Meningitis Diagnosed?
After visiting a healthcare provider, they’ll take a medical history and do a physical exam to determine if meningitis is a possibility, Dr. Schaffner says. They may also do a blood test, which can help determine how severe the infection is and what might be causing it.
But the only definitive way to diagnose meningitis is via a lumbar puncture, he says. A physician will insert a needle between two vertebrae to collect cerebrospinal fluid, which will then be sent to a laboratory to test for the bacteria that can cause meningitis, Dr. Schaffner says.
A lumbar puncture can rule out other causes for the symptoms, such as viral meningitis, he says. It can also help determine the type of bacteria that’s causing the meningitis, which can help your medical team choose the best targeted treatment.
Since meningitis moves so quickly, while you wait for those results to come back your physician will likely begin you on antibiotics — the standard treatment for bacterial meningitis — and set up supportive care, such as an IV, blood pressure monitoring, and breathing support if needed, he adds.
How Can You Prevent Meningitis?
“Prevention is where we have the gold star,” Dr. Schaffner says. “There are vaccines that will prevent these kinds of meningococcal infections, and as a consequence, this very scary kind of meningitis, which when I was a younger physician was moderately common, is distinctly rare now in the United States. That’s a terrific advance, and it’s related entirely to the development of effective vaccines and their widespread implementation.”
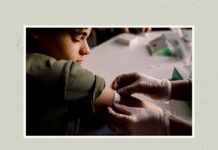
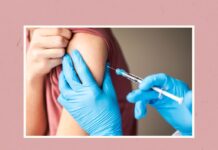
There’s a meningitis vaccine (the pneumococcal vaccine) that’s given to infants, but for teens, the meningitis vaccine that’s most widely recommended is MenACWY, which protects against four serogroups (types) of bacteria. There’s also the MenB vaccine, which protects against serogroup B, a type of bacteria that’s responsible for about a third of all cases of meningitis in the U.S., per the National Meningitis Association.
Since the MenB shot only gives short-term protection (about a year or two), the CDC only recommends it for certain high-risk groups. But anyone between ages 16 and 23 can receive it if they and their healthcare provider decide they’d benefit, and Wukovits stresses the importance of doing so.
Dr. Nachman also suggests speaking to your child’s school and asking if there have been any recent outbreaks and if they recommend or require any specific vaccines.
But vaccines don’t protect against every strain of meningitis. So in addition to vaccination, knowing the symptoms of meningitis and what to do if you notice them is key. Since meningitis progresses so quickly, getting help and starting treatment as soon as possible can help improve outcomes.