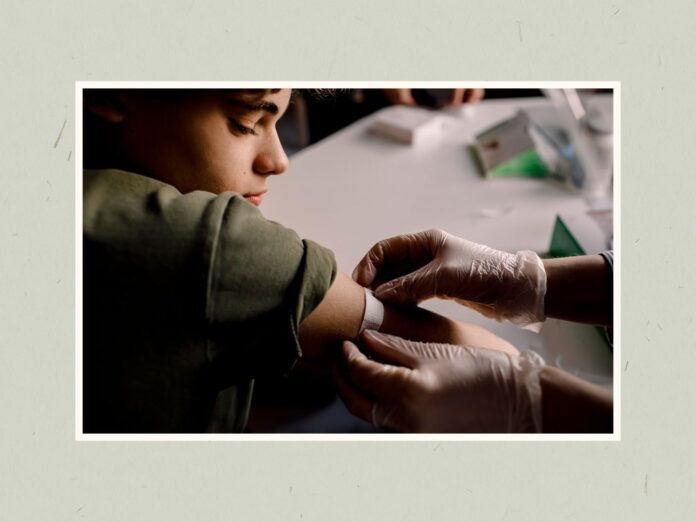
Between rampant myths about vaccine safety and competing guidelines for pediatric vaccines floating around on the web, it’s easy to see why parents might be confused about what shots their kids need and when. But when it comes to meningitis, vaccines are critical. Here’s everything parents need to know about this rare and potentially life-threatening infection.
Meningitis occurs when the thin membranes surrounding the brain and spinal cord become inflamed as a result of a bacterial or viral infection that enters a person’s bloodstream. It’s deadly in roughly 10 percent of all cases.
“It’s scary and important to think about,” Elizabeth Murray, DO, MBA, pediatric emergency medicine doctor, tells SheKnows. However, thanks to modern medicine, “it’s not an overly common medical problem.” So, if your young child or teen is up to date on their vaccinations, and there aren’t any known outbreaks in your area, then there’s no need to panic.
Bacterial meningitis is usually the type of outbreak we hear about in the news — it’s often the most contagious and rapidly fatal, whereas viral cases tend to be less serious. Per Mayo Clinic, the germ Streptococcus pneumoniae, or pneumococcus, is the most common cause of this condition in babies and young children. It can also stem from a more contagious bacterium called Neisseria meningitidis, or meningococcus, which is known as meningococcal meningitis. Exposure to meningococcus doesn’t always result in meningitis; in fact, about one in 10 people have this bacterium in their mouth or nose and never fall ill. But when it does lead to an acute illness? Things can go downhill fast.
According to the Centers for Disease Control and Prevention (CDC), meningococcal disease can affect anyone at any age, though rates are highest in babies under the age of 1. Teens and young adults ages 16 to 23 are also at a higher risk, particularly those who live in communal settings like college dorms or military housing, where germs that can cause meningitis spread quickly through close contact.
Whether bacterial or viral, meningitis requires quick diagnosis and treatment. However, in the early stages, “it can be very difficult to detect because the symptoms are very similar to any other infections, like a fever or feeling lethargic,” Catherine Mary Healy, MD, pediatrician and member of American Academy of Pediatrics’ (AAP) Committee on Infectious Diseases, tells SheKnows.
If meningococcus is the root cause, a young child might present with a red or purplish rash that doesn’t fade when you apply pressure, Healy explains. They might also be feverish, extremely irritable, stiff, or develop a tense, bulging spot on their head. Other meningitis symptoms include severe headaches, light sensitivity, and a stiff neck. Bacterial cases are treated with antibiotics; depending on severity, viral cases can be treated with antiviral medications or left to run their course. In severe cases, this condition can cause seizures, long-term disabilities, or even death.
The good news? As scary as it sounds, meningitis is largely preventable thanks to vaccines, which protect kids from harmful bacteria and viruses. These shots are so effective that they’ve drastically reduced rates of meningitis worldwide.
For babies, the AAP, the nation’s largest organization of pediatric health experts, universally recommends two vaccine series for meningitis: the pneumococcal vaccine, and the haemophilus influenzae type B (HIB) vaccine. (Don’t let the name confuse you; the latter shot has nothing to do with the flu.) For all preteens and teens, the AAP recommends the meningococcal vaccine (MenACWY), administered around ages 11 to 12 and again at 16. As the name suggests, it specifically protects against meningococcal meningitis.
The meningococcal type B vaccine (MenB), which targets a specific strain of meningococcus, is also available at ages 16 to 18 through shared clinical decision-making — in other words, parents and healthcare providers making informed choices together. This shot offers fuller protection for young adults who live in congregate settings. For children and teens who have a weakened immune system or other risk factors, providers may recommend additional boosters.
Meningitis is one condition that could become more common if vaccination rates drop, Murray cautions. That’s why following the AAP’s pediatric vaccine schedule — which extends well into your kid’s high school and college years! — is key. Beyond the aforementioned shots, “many childhood vaccines protect against germs that can cause viral meningitis, like chickenpox,” she explains. “The timing of vaccines is very important. The recommendations are based on a combination of the best timing based on risk, and best timing based on a child’s immune system development and ability to respond to the vaccine.”
Routine prenatal care is also an important preventive measure, Murray adds. Pregnant mothers can unknowingly pass on germs like herpes simplex virus (HSV) to their babies during or near delivery. This can cause a particularly deadly form of meningitis.
That’s a lot to remember, so here’s the main takeaway: Vaccines are your kid’s best defense against meningitis. If you have specific questions, talk to your family’s pediatrician. They should be your go-to resource for accurate, science-based information about what shots your kid needs for vaccine-preventable illnesses. Healy also recommends asking your provider if your child “has any of the risk factors putting them in the group for whom [additional] vaccination is recommended” for meningococcal meningitis.
And if you’re at all concerned that your young child or teen may have meningitis? Take them to the doctor right away. “It’s always important to remember that infants less than 60 days old should be evaluated anytime they have a fever,” Murray says.